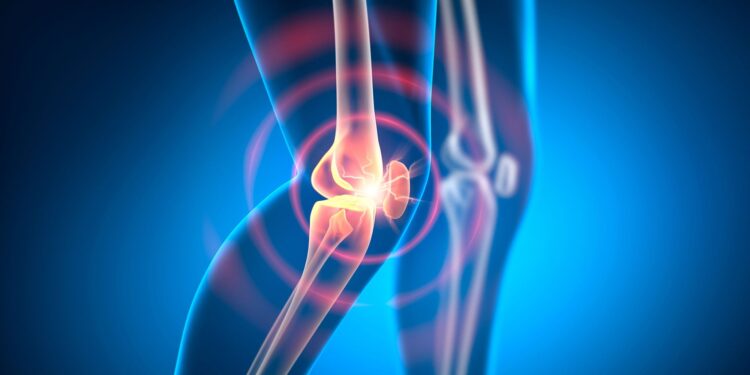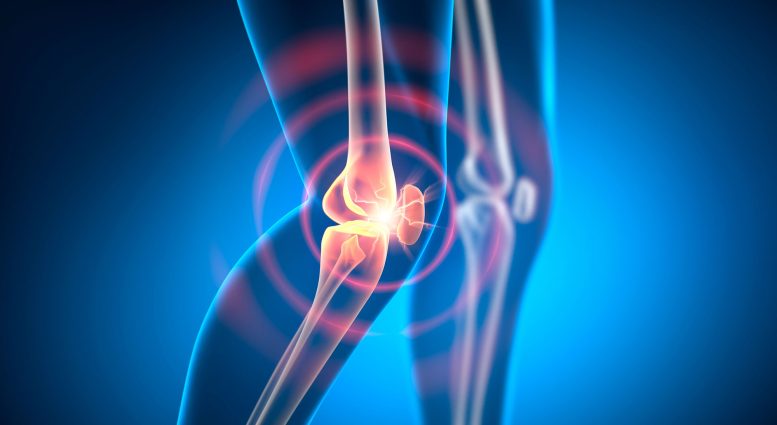
Scar-driven adjustments in joint tissue could underlie therapy resistance in rheumatoid arthritis, opening the door to new focused therapies.
Rheumatoid arthritis (RA) impacts tens of millions worldwide, inflicting persistent joint ache, swelling, and stiffness when the immune system mistakenly assaults the tissue lining the joints.
Over the previous 20 years, an increasing toolkit of anti-inflammatory and immune-targeting medicine has remodeled care, but a considerable subset of sufferers nonetheless don’t obtain remission, even after attempting a number of therapies. For these people, ongoing signs will be debilitating, and clinicians have restricted steerage on what, biologically, is driving the cussed illness that is still after irritation is introduced underneath higher management.
In a brand new Nature Immunology paper, Mass General Brigham researchers Kevin Wei, MD, PhD, and Kartik Bhamidipati, PhD, tackle that drawback by trying past broad immune alerts and into the structure of diseased tissue itself. Their workforce used next-generation mapping instruments to see the place particular cell sorts sit, how they work together, and the way these relationships shift earlier than and after therapy, capturing the joint microenvironment in unusually excessive decision.
Their findings level to an important, and doubtlessly targetable, piece of the treatment-resistance puzzle: fibroblasts and scarring pathways that seem to persist even when irritation is introduced underneath management. By revealing how disrupted cell-to-cell communication and wound-healing alerts could drive ongoing tissue injury and ache, the work helps clarify why some sufferers don’t get higher with at the moment’s anti-inflammatory methods alone.
Within the Q&A under, Wei and Bhamidipati talk about the unmet scientific want, the spatial transcriptomics method that made this doable, and what these insights might imply for extra exact therapies for sufferers who’ve run out of choices.
What challenges or unmet wants make this examine vital?
Rheumatoid arthritis (RA) is a standard autoimmune illness the place the physique’s immune system mistakenly assaults the liner of its personal joints, inflicting continual ache, swelling and stiffness.
Whereas there have been exceptional developments within the therapy of RA with an array of therapies that concentrate on irritation, a big subset of sufferers (roughly 6-28%) proceed to expertise difficult-to-manage signs of illness even after receiving a number of traces of therapy. There’s a essential have to establish new therapeutic approaches for sufferers who’re refractory to current therapy choices.

What central query(s) had been you investigating?
Our analysis centered on discovering why some individuals with rheumatoid arthritis don’t reply properly to plain remedies, by trying carefully on the biology of their joint tissue.
What strategies or method did you utilize?
We noticed an exaggerated wound therapeutic response (fibrogenesis) within the joints of sufferers who failed to attain remission. Although the remedies had been efficient in depleting immune populations and lowering joint swelling, they weren’t adequately efficient at assuaging joint ache in non-remitting sufferers, which was linked to elevated tissue scarring.
We additionally found that the buildup of scar tissue in joints occurs as a result of the conventional communication between blood vessels and endothelial cells with close by assist cells, referred to as fibroblasts, will get disrupted. If we are able to discover methods to assist these cells speak to one another correctly once more, we would be capable of cease and even reverse the dangerous scarring that results in ongoing joint issues.
What did you discover?
We noticed an exaggerated wound therapeutic response (fibrogenesis) within the joints of sufferers who failed to attain remission. Although the remedies had been efficient in depleting immune populations and lowering joint swelling, they weren’t adequately efficient at assuaging joint ache in non-remitting sufferers, which was linked to elevated tissue scarring.
We additionally found that the buildup of scar tissue in joints occurs as a result of the conventional communication between blood vessels and endothelial cells with close by assist cells, referred to as fibroblasts, will get disrupted. If we are able to discover methods to assist these cells speak to one another correctly once more, we would be capable of cease and even reverse the dangerous scarring that results in ongoing joint issues.

What are the real-world implications, significantly for sufferers?
Our examine identifies one of these tissue scarring as a key driver of treatment-refractory RA. This mechanism stays unaddressed by the present therapeutic panorama and affords a novel, targetable pathway for sufferers immune to current remedies.
What rising tendencies on this subject excite you proper now?
Advances in expertise are dashing up the deep molecular profiling of affected person samples, ushering in an thrilling period of precision drugs for autoimmune ailments the place therapy is tailor-made to a affected person’s distinctive molecular traits (corresponding to protein ranges, enzyme exercise, and extra).
This focused method guarantees to switch the present trial-and-error therapy strategies with more practical interventions, considerably bettering affected person outcomes and high quality of life.
Reference: “Spatial patterning of fibroblast TGFβ signaling underlies therapy resistance in rheumatoid arthritis” by Kartik Bhamidipati, Alexa B. R. McIntyre, Shideh Kazerounian, Gao Ce, Quickly W. Wong, Miles Tran, Sean A. Prell, Rachel Lau, Vikram Khedgikar, Christopher Altmann, Annabelle Small, Roopa Madhu, Sonia R. Presti, Ksenia S. Anufrieva, Philip E. Blazar, Jeffrey Okay. Lange, Jennifer A. Seifert, Accelerating Medicines Partnership RA/SLE Community, Accelerating Medicines Partnership: Autoimmune and Immune-Mediated Illnesses Community (AMP-AIM), Colorado Interdisciplinary Joint Biology Program (CUIJBP) Consortium, Larry W. Moreland, Adam P. Croft, Melanie H. Smith, Laura T. Donlin, Myles J. Lewis, Anna H. Jonsson, Costantino Pitzalis, Ranjeny Thomas, Ellen M. Gravallese, Michael B. Brenner, Ilya Korsunsky, Mihir D. Wechalekar and Kevin Wei, 15 January 2026, Nature Immunology.
DOI: 10.1038/s41590-025-02386-2
This work was supported by grants from the National Institutes of Health (NIH-NIAMS K08AR077037, NIH-NIAMS T32AR007530-36) and the Burroughs Wellcome Fund Career Awards for Medical Scientists.
Disclosures: Wei has a sponsored-research agreement from Merck Pharmaceuticals, BMS, Anaptys Bio and 10x Genomics.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.